
Close

Subscribe to out newsletter today to receive latest news administrate cost effective for tactical data.
96 Clinton Ave, Newark, NJ 07114, United States
Certified specialists manage claims, coding, and denials to maximize reimbursements and free your time for patient care.
Request Free Consultation


500+ Physicians
40+ Specialties

Medical Billers & Coders

RPA Billing Solutions

Clean Claim Rate
Transcure’s intelligent RPA platform applies 4M+ compliance rules to boost accuracy, achieve 98% first-pass acceptance, and accelerate payments — freeing your staff to focus on patient care.

We use cutting-edge tools to improve billing accuracy, automate workflows, and reduce errors..
Read More
From claim submission to collections, we handle the full cycle for maximum reimbursements..
Read More
Our solutions adapt to any practice size, ensuring performance and supporting growth..
Read More
Built-in tools detect and fix issues early, reducing denials and payment delays..
Read More
We streamline operations to speed payments and strengthen your financial stability..
Read More
We keep you HIPAA-compliant, safeguard data, and minimize regulatory risks..
Read More
Access real-time insights to track trends and make data-driven decisions..
Read More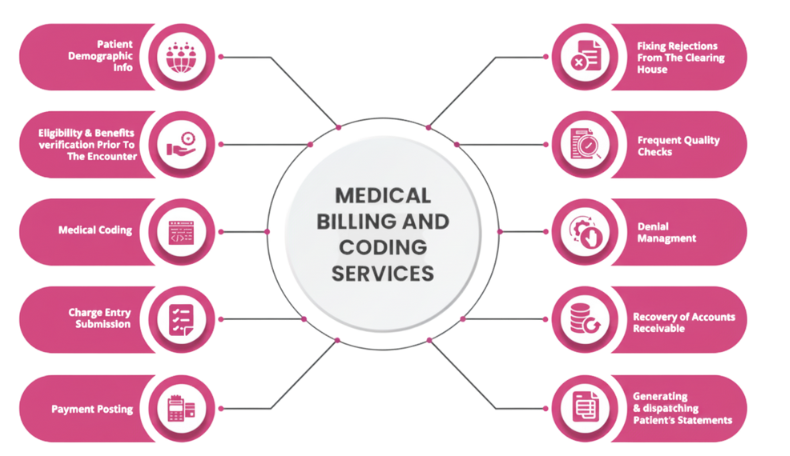
Medexa RCM delivers tailored billing solutions for primary care, specialty clinics, and surgical centers — ensuring accuracy, faster reimbursements, and HIPAA compliance.













Medical billing is the process of submitting and following up on claims to health insurance companies to get paid for medical services. This process is complex and involves several steps, starting with patient registration, demographic entry, and insurance verification. Once those steps are complete, the process moves on to charge entry where services are added, then medical coding, where medical procedures are translated into CPT and ICD-10 codes. Then claim submission where the coded claims are sent to insurance for payment.
Our fee is a transparent starts from 2.99 % of net collections—no hidden charges.
We import your payer rules, set up ERA/EFT, and go live in 14 days.
Revenue cycle management (RCM) is the total process of managing the finance of a healthcare organization from patient registration to payment posting. This complex process has many steps, including managed billing, charge capture, coding and insurance verification. Effective RCM allows healthcare facility providers to have an improved cash flow, reduce administrative burdens and optimize their finances. By managing the entire revenue cycle, healthcare specialists can focus more on patient care while keeping their financial house in order.
Medical billing is the process of submitting and following up on claims to insurance companies to get paid for services rendered by healthcare providers. It’s a big part of the revenue cycle and directly affects the financial health of medical provider.
We handle claim denials by thoroughly analyzing the root cause, correcting errors, and promptly resubmitting the claims. For appeals, we gather necessary documentation, follow payer guidelines, and advocate for accurate reimbursement.
Yes, absolutely! We utilize real-time claim scrubbing software to identify and rectify errors before submission. By addressing incomplete information, coding errors, and insurance verification processes, we can streamline billing and improve efficiency.